
This past year has been a wild ride for me. About a year ago on a random Tuesday morning, I woke up, sat on the toilet, realized things “down there” didn’t feel quite right, and had a mild panic attack. I think my exact words were, “Wow. Holy S@$*t! My uterus is falling out of my body!!!!!”
Remember back five years or so ago when I wrote that I had a “tilted uterus” and that it was a very common after effect of pregnancy? That it wasn’t harmful, but only affected how I need to insert my menstrual cup? That its only real side effect was a tiny bit of urinary incontinence when I did sports? What I didn’t know then (and what I wish I’d known) is that a tilted uterus isn’t a thing, medically speaking. It’s actually a condition known as pelvic organ prolapse, and if left untreated it only gets worse.
In fact, it can often require major surgery — surgery which uses a controversial treatment of mesh slings to hold your pelvic organs in place. There are three major types of pelvic organ prolapse: uterine (uterus collapse into the vagina), cystocele (bladder collapse), and rectocele (colon collapse).
Me? I’ve got all three!
How did it get to this point? Based on all the reading I’ve done in online support groups and message boards for women with pelvic organ prolapse, my story feels very common.
According to the National Institutes of Health, 24% of all U.S. women currently have pelvic organ prolapse and 50% of all women over 80! (source)
If it’s so common, why aren’t we talking about it? Why did it take my by surprise?
And more importantly, is there something I can do to keep it from taking you, my dear readers, by surprise?
Pelvic Organ Prolapse: Symptoms I’d Wish I’d Known Weren’t “Normal”
Until this year, I’d been told by multiple doctors, physiotherapists, nurses, and other lady friends that the below symptoms are very common post-birth and are really nothing to worry about.
They were wrong! These symptoms don’t exist in a vacuum and almost always reveal themselves as part of a larger problem.
1. Urinary Incontenence
It started after the birth of my second baby. I’d run across the street and pause in horror on the other side when I realized the jogging had cause a little squirt of pee to come out. Oops!
I’d jump on the trampoline with my kids and accidentally piss myself.
From everything I’d read online to all the friends I’d confided to in person, the consensus seemed to be that this is normal post-birth and that the solution is simple: do pelvic floor exercises to strengthen your pelvic floor.
So I started doing my kegels religiously, tried to get into routines of doing squats and lunges and using my fitbit, and even invested in a treadmill desk.
It helped! My incontinence became a little more rare. But I was still looking at it as if it were the only problem and exercise the solution.
This past January, my “solution” stopped working. My incontinence grew suddenly worse.
Now I would piss myself when I sneezed or coughed, and not just occasionally, but EVERY. SINGLE. TIME.
I now know that my incontinence was getting worse because my “tilted uterus” was actually falling into my bladder, pushing my bladder lower and lower until now it’s almost fully collapsed!
In fact, all that exercise probably made my prolapse worse. As any lady with pelvic organ prolapse will tell you, once you have prolapse, most “normal” exercise (think squats, lifts, running, sit ups, etc) only exacerbates the problem. Instead, you have to switch to special exercises that have been approved by a licensed Pelvic Floor Physiotherapist.
2. Constipation
Generally speaking, my body’s always erred on the side of constipation. I’ve long assumed it’s kinda normal, just how my body’s internal chemistry works out.
My go-to solution is and has always been to supplement with magnesium. I even make my own magnesium oil so it’s cheaper.
Does it help? Yes.
Did it keep me from realizing that my constipation was actually caused by my colon collapsing into my vagina? Yes!
3. Back Pain
Again, I just assumed it was from lack of proper exercise. Maybe I needed to replace my mattress (here’s the non-toxic one I bought) or ground myself when I sleep.
I started getting routine massages, like religiously.
Now I know that this mild back pain was actually being caused by my pelvic organs all falling out of place. (They’re basically a pile of mush down there. Ugh!)
4. Reduced Sexual Sensitivity.
As embarrassing as all this is, it needs to be said. One of the earliest symptoms of prolapse I can remember, second only to feeling my cervix in the wrong place and being told that it was “just” a tilted uterus, is that sex felt … different.
Once again, when I brought it up with the gynecologist who fitted me for my diaphragm (sorry! This whole post is feeling a bit TMI at the mo), she told me it was normal.
She said that it’s common for the vaginal walls to be super stretched if you’ve had children, and for that to cause decreased sensitivity during intercourse. Nothing to worry about. Just focus more on clitoral stimulation, and you’ll be good to go.
In fact, while it is normal, it’s also a common symptom of pelvic organ prolapse.
All of these symptoms are “normal,” if you define normal as something fairly common to the average woman.
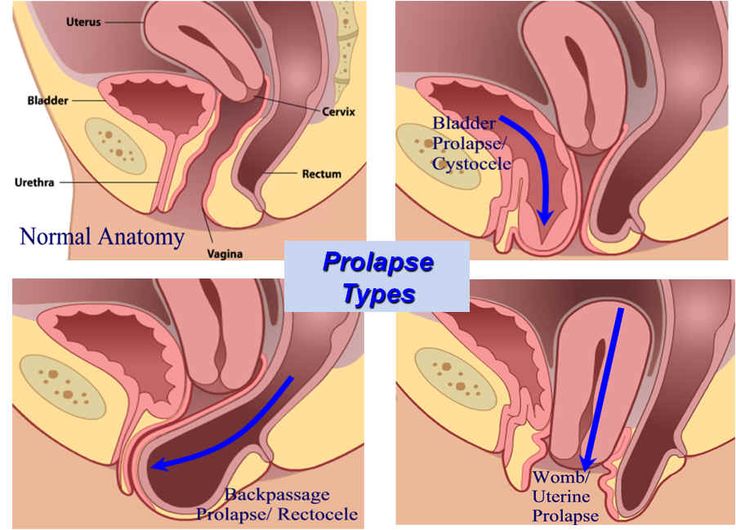
Yes, it’s all normal! But so is Pelvic Organ Prolapse.
Here’s the deal, ladies.
Pelvic Organ Prolapse is normal. It will affect half of all women in the course of their lifetime. (source)
It affects nearly 1 in 4 of all women post-birth, and once they hit menopause, the numbers keep rising.
Sadly, doctors are used to thinking of it as a condition of aging, so when a younger woman comes in with all the same symptoms they tell her she’s fine … until she’s suddenly not fine and actually needs surgery.
I’m trying to avoid surgery. Here’s what seems to help.
The first thing you absolutely must do is visit a urogynecologist. Not a gynecologist. Not a urologist. A urogynecologist. They are the only medical professional who specializes in pelvic organ prolapse, and they are the only ones who can give you a clear diagnosis.
If you try going to a gynecologist, they won’t be on the lookout for prolapse. In fact, the last time I went to one I had multiple stage 2 prolapses and they told me everything was fine down there. That’s because they did my exam with me on my back and my feet in stirrups.
A proper exam for prolapsed organs is done with the patient standing up and/or squatting, FYI.
Once you get your diagnosis, here’s what can make living with prolapse more manageable:
1. Get Fitted for a Pessary
Pessaries are devices that get inserted into the vagina and hold everything in place.

They have a long, weird history. “In fact, the problem of uterine prolapse and its potential treatment is described in the oldest documented medical literature, the Egyptian Papyri, where it is written, ‘of a woman whose posterior, belly, and branching of her thighs are painful, say thou as to it, it is the falling of the womb,'” (source). In ancient times, treatment for prolapse included everything from succussion (see drawing) to leg binding. Eventually pessaries started being used. Originally, they seemed like nothing less than torture devices. Bronze, inverted cone shaped pessaries with perforated circular plates? No thank you! (source)
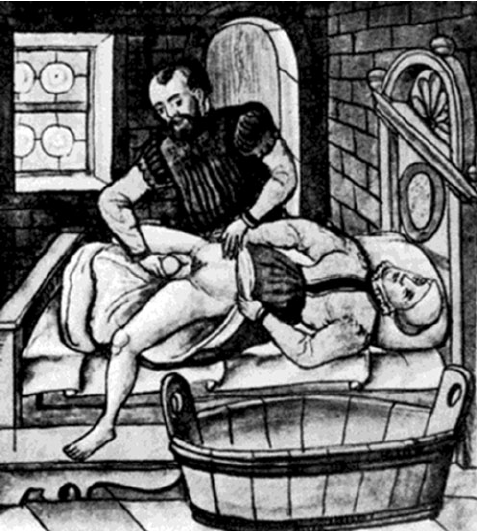
They eventually evolved into more comfortable models like wine-soaked wool that had been wound up and tightly compressed or vinegar-soaked sea sponges that had been shaped to insert. (source) Even pomegranates were halved and inserted to try to keep internal organs from falling out! (source) In the 16th century, Ambroise Paré, the royal surgeon who treated no less than 3 kings during his lifetime, invented the pre-cursor to the modern pessary for the queens and queen mothers under his care.
These days, pessaries are made of medical-grade, non-irritating silicone. A well-fitted one is comfortable, allows for freedom of movement (including squats!), keeps all your pelvic organs from further succumbing to gravity, and can be worn during bowel movements. Many types can even be worn during sex.
I have a couple of pieces of advice for any of you ladies who need a pessary.
First, if at first you don’t succeed, try and try again! It took me three attempts to get a well-fitting pessary, and each attempt before the last was more and more discouraging.

You see, pessaries come in all sorts of shapes and sizes. They can range in size from a few centimeters wide to a few inches wide. Different shapes are better for different types of prolapse. And some have clear advantages (like being able to stay in during sex!).
Some urogynecologists are stuck on one type over another, with the hands-down favorites being a ring pessary (the top row) or the gellhorn (second from the left on the bottom row.) As my luck would have it, neither of those was particularly good for my multiple stage-3 pelvic organ prolapses.
I eventually settled on a cube pessary (3rd one, bottom row) and insert it every time I need to be active. It’s very easy to insert and remove (particularly if you have any experience with inserting or removing menstrual cups).
Second, don’t be afraid to experiment! I tried out quite a few new things before I settled on my cube pessary. For example, did you know you can still buy sea sponges to hold your uterus in place? A number of women completely swear by them, saying that once you figure out how to trim them to the right size, there’s absolutely no pessary more comfortable than a sea sponge.
(Click here to buy a sea sponge pessary on Amazon!)
Of course, my prolapses were bad enough that a sea sponge is not adequate. I needed something more durable and firm that I could insert higher into my vagina.
And, I still want to try the Inflatoball, which is only available for purchase from the UK and Europe (what’s a little extra VAT compared to the value of a more comfortable life?). One of these days, I’m going to buy it and try it.
My point? It’s easy to get discouraged when trying and failing to find solutions. It’s easy to give up and resign myself to surgery, but I believe the key to living successfully with pelvic organ prolapse is experimentation and optimism.
2. Switch Your Exercise Program
As I said above, most standard exercises can make your prolapse worse. If I had known this years ago, I firmly believe I could have stopped my prolapse in its tracks before it progressed further.
Basically, it’s really important to avoid most full-body exercises. Any exercise that increases pressure on the abdominal area will exacerbate your pelvic organ prolapse. (source) Think sit ups, leg lifts, dead lifts, planking, push-ups, etc. Even walking or running (especially without a pessary to support your pelvic organs!) can make stage 2 or 3 prolapses worse. (source)
It’s important to use specially designed exercises that either isolate your pelvic floor muscles or isolate your other muscles away from putting pressure on your pelvic floor.
A Pelvic Floor Physiotherapist is a must for teaching you these exercises. If your insurance doesn’t cover one, you may find yourself in the same boat I was in — desperately searching YouTube for pelvic floor friendly exercise programs.
Mostly, you’ll find a lot of individual pelvic floor physiotherapists selling their own online exercise program. I’ve evaluated a half dozen of them now, and I’m most impressed with the MUTU system! They have a FREE 30 Day Pelvic Floor Challenge that you can sign up up for which uses a 6-minute daily workout as the baseline. (Click here to sign up for the FREE challenge!)
3. Use a Kegel Toner
So, I know this sounds like a joke. I thought it was super weird at first, too. But now it’s definitely my favorite thing to have bought so far this year.
Studies have long shown that pelvic floor exercises (like kegels) are good at reducing pelvic organ prolapse severity and symptoms. (source) (source) (source)
But what they don’t tell you, at least in the US, is that a kegel can be done more efficiently with the use of electronic muscle stimulation. (source) (source)
In fact, over in the UK and a significant part of Europe, kegel devices are commonly prescribed to patients with incontinence. My UK lady friends were all shocked that it wasn’t my urogynecologist’s first recommended treatment method.

I recently purchased the K-Fit Kegel Toner. On average, when you do a kegel without the aid of a device, you probably flex about 40% of your pelvic floor muscles. According to the K-Fit manufacturer, with the aid of their device, it increases to about 90% efficacy.
I’ve been using it now for nearly 6 months, and I have seen results! Not only have I been able to increase the strength and length of the exercise program I’m using, but I no longer have stress incontinence!! I don’t accidentally pee on myself when I sneeze or cough. And, with time, I’ve noticed my cervix resting higher in my vagina, too.
(Click here to buy a K-Fit Kegel Toner!)
The most important thing to remember when it comes to using a kegel toner is to put the nodes horizontally instead of vertically (stimulating the sides of your vaginal opening rather the front and rear). If you position it wrongly, it will feel like it’s “pinching” your bladder and rectum — an uncomfortable situation, to say the least.
4. Use Estrogen Cream
Now, I’m not sure how important this is, but the studies seem to show that a drop in estrogen levels weakens the vaginal walls (allowing uterine prolapse to get worse). (source) It is recommended that you use a topical estrogen cream, specifically to insert and remove your pessary and to massage into your vaginal walls daily because it’s more effective than oral hormone pills. (source)
This was an especially hard treatment for me to accept because in all other areas, I showed signs of estrogen dominance. What I can definitely say after 6 months of daily use is that this did not worsen my estrogen dominance symptoms.
After some research, I decided to go with BioLabs PRO BioEst 2.5 bioidentical estrogen cream. It uses both Estriol and Estradiol, so it has your bases covered. And I don’t need more than a pump in the morning massaged into and around my pelvic floor and a pump to lube up my pessary per day.
(Click here to buy BioLabs PRO Bioidentical Estrogen Cream)
Pelvic Organ Prolapse Resources
After my panic attack moment last year, I did a small amount of research over the course of a week and realized I had Pelvic Organ Prolapse. I also realized that not many women talk about it openly because it’s such an embarrassing topic.
I joined the Association for Pelvic Organ Prolapse Support (APOPS) and read a ton of their articles. I even joined their private Facebook group so that I could talk to women who were experiencing the same thing as me. Those online forums have been a life saver!
It’s also made me realize that I don’t have it as bad as many other women. Despite severe, multiple prolapses, I’m not in inexplicable disabling pain, nor do I have a job that requires me to be on my feet all day. The symptoms I highlighted today are just the tip of the iceberg, a mere introduction to a topic that is wide and deep and has thousands of articles about it posted online.
If you suspect you may have pelvic organ prolapse, feel free to leave a comment below and I will do my best to answer your questions, commiserate with you, and/or steer you in the right direction for finding the medical help and resources you need!
Featured Photo by Victor Freitas from Pexels
 |
















Thank you for bravely sharing your story and resources. You are so right that nobody talks about this, yet it’s so important to know. Many women will now benefit from your willingness to be vulnerable. Thanks you!
Thank you for the encouraging words! All the best, ~Kristen
You have to check out Kimberly Ann Johnson’s work. She has a great podcast about *healing* Not managing pelvic organ prolapse without surgery.
Thanks, Rachel. I’ll definitely check it out! Cheers, ~Kristen
ok, this terrified! I do crossfit almost daily and I love it, but I’m going to look into this. My sister told me a few months ago that Mom’s “bladder dropped” and she had some device or surgery. (She passed away a decade ago so I have no idea how long ago or what treatment was back then.) Since I have a tilted uterus and some of these issues now that I’m in menopause, I will investigate this. Thank you so much for sharing! You always have the most helpful articles.
It sounds like you may be in the early stages of prolapse! If I were you, I’d definitely make an appointment with a urogynecologist to get a diagnosis so I could start doing early physiotherapy.
I had all of the prolapses as well, including a couple of rectocele’s. I worked with a therapist on the special toning exercises for a while, and it helped a bit… But not enough. I finally was fitted for a pessary… which was great, everything felt like it was back in place, but it made my urinary incontinence so much worse. I am actually had the surgery and was going to get the mash but at the last minute my husband who is a surgeon, convinced me not to. I do have a sling for the urinary incontinence, no mash, and they repaired all of the prolapses which included lifting my bladder and sewing it to tissue above. Also had a partial hysterectomy at that time. Recovery was a bit rough for the first two weeks, however it’s sold all my issues and I’ve had no problems since, which has been five years 🙂
It’s my understanding that if a pessary makes your symptoms worse, then it’s just not the pessary for you. I had one that made me feel like I had an overactive bladder (constant urges to pee) every time I stood up, so I nixed that baby and got a totally different shaped pessary that not only fits but helps all of my symptoms. Congrats on your surgery working out so well! Cheers , ~Kristen
hi Kristen,
Sorry to hear about your situation. I have seen a number of women with this kind of problem. Homeopathy can be extremely helpful in supporting self-healing. The first remedy that comes to mind is Sepia. There are other remedies. Homeopathy seeks to individualize the remedy with the person who has the complaint but for many many women, Sepia is likely to help relieve.
Wishing you speedy healing so that you can live life with sneezes and laughter without worrying about leakage!
I will definitely look into it! You are the second person to mention it to me since I wrote this post. Thank you! ~Kristen
I have found a Physical Therapist who studied under the Barral method, and she is a magic worker! She is my lifesaver! I also see a gentleman named Frank Lowen who also studied under Barral and then branched into his own system called “The Lowen System”.
These two are awesome! I would suggest looking up Barral on google and see if you can find someone who follows his methods.
I will definitely look into it! Thank you for the recommendation. Cheers, ~Kristen
It makes me super upset to hear that doctors told you all of this was normal.
It is NOT normal to have weak pelvic muscles.
It is NOT normal to have reduced sensitivity after pregnancy due to intercourse.
It is NOT normal to not be able to feel your pelvic and vaginal muscles in general!!!!
These muscles are like any others in the body – they need to be strengthened and kept in shape to work. These are also the muscles that aid a woman during labor to push a baby out, and they don’t get ‘stretched out’ and never go back to shape. That’s crazy talk. They’re meant for this job, and they need attention and care like any other muscle.
You may want to check into a jade egg practice with weights. This is along the lines of kegels, but with an important distinction: it’s training the muscles. Often, kegels are just advertised as a squeezing action. Well, think about it – if you go to the gym and just squeeze your biceps, they’re not going to get stronger. You need to have a dumbbell in your hand.
It’s not any different here.
They sell jade eggs that have a drilled hole (be careful of substances other than jade, because they tend not to be super strong) and then you can thread unwaxed floss through it and hang small vaginal weights off of it.
Layla Martin and Kim Anami have a lot of practices online that you can purchase so you’re doing things the right way. I can’t speak to others because some of them recommend just putting the jade egg in, which doesn’t do much and is not the point.
Anyway, Kim also has little video segments about all of her tantra practices. She’s more expensive than Layla’s courses, but I love both of these ladies. They are funny, they are sincere, and their content has nuts and bolts to it so you can learn about how to take care of yourself.
I’m honestly very tired of doctors shying away from sex in general and treating women like their sexual health and its pleasure and strength aren’t important. It’s absolutely ridiculous, and as you can see, is also affecting us adversely all across the board when it comes to urinary problems and the like. Puritanical culture, and frankly, the birds and the bees are not that big of a deal. It’s a fact of life.
I already follow Layla Martin, so I’ll look into Kim Anami. Thanks for sharing! ~Kristen
I am so grateful you gave us this information. This is my situation exactly, now 64, and they were telling me the same thing my whole life: tilted uterus, peeing when playing sport, etc. Thank you for being specific about the “urogynocologist”.
It’s really infuriating to be told over and over again that it’s normal, only to find out later that it can lead to some very bad, debilitating things if you don’t nip it in the bud! Cheers, ~Kristen
Thanks for all the great information, Kristen! I appreciate your willingness to share personal facts so openly. I believe more woman have similar types of things happening with their bodies and the solutions they’ve been given are not necessarily appropriate. I’ve learned so much from this blog and will be looking for a urogynecologist to sort this all out – THANK YOU!!!
You’re so welcome. It was a bit scary to write, but I felt compelled to say something about it because I had been so ignorant myself. If I can save even one person from making the same mistakes I did, it’ll have been worth writing! Cheers, ~Kristen
Thank you for this information as it is priceless. I had a 3 lb tumor removed about 8 years ago. They ended up taking everything leaving mounds of scar tissue. When I went in for my GYN appointment I cried throgh the whole thing. It really hurt and I am not a baby…I can take pain. They had to force open my vagina with metal speculum which was horrific, so they could go in and get a culture. P>S> scare tissue does NOT stretch… I VOWED never to have this done again. I cried out the whole time, she thought I was being a baby. (never saw her again) So I am wondering if it can still prolapse even with all the scar tissue? I am 67 now and starting to pee a little when I sneeze, not all the time but sometimes. I want to get ahead of the game.
You are helping so many women…you have no idea. Thank you again we all appreciate your candor and we highly respect you.
If I were you, I’d definitely find a urogynecologist and make an appointment! As far as I know, then answer is yes. You can definitely prolapse even with scar tissue, even post-hysterectomy, etc. Talk to someone who specializes in prolapse, and you’ll have your answer. Cheers, ~Kristen
What if you have never had children? Do the same exercises and treatments apply? Would the MUTU system help or not?
Yes. MUTU is marketed for moms, but I found the exercises to be pretty universal.
So women who never had children can still get one or more of these types of prolapse? Since menopause, a few times a year, I pee a little when I sneeze. I’ve also noticed that my vulva is sagging a bit, but I figure that’s gravity and aging at work. I’m wondering if I should be more proactive or not worry.
Yes, while it’s common in post-natal women, it’s most common in women after menopause. If I were you, I would talk to a urogynecologist soon!
Sorry, but those Kegels are probably what caused the further problem. Check out Katy Bowman, a biomechanist, that actually specialized in pelvic floor issues in college.
And I”m sorry if that sounded rude, I just re read my comment, and it might. But seriously, Katy has free info and vids up the wazoo online and what she’s teaching is a science based (mechanics and physics) practical series of expertises and methods (posture does not equal alignment) and is literally saving my body from collapse. She’s up the with the Gokhale Method and Ida Rolf.
Helena, I’ve been a fan of Katy Bowman’s for a while now too and first found her for pelvic floor stuff. But I’ve also not made much progress as a result. I find her information *so* vast and scattered that it’s hard to figure out exactly where to start especially if you have a specific goal. Do you have recommendations of where to start to really make a difference on specifically pelvic floor and internal organ alignment improvement? I’ve also been looking for a place where people might be chatting or sharing about her ideas and recommendations — do you know of one? For example — she has her “lists” of minimalist shoes on her website, but doesn’t respond to specific questions about circumstance. I’m wondering if others have experience on — for example — which shoes work for kids with hypermobility and hyperlax ligaments in their feet and ankles, and if there are any circumstances at all when strengthening muscles isn’t enough and an arch support is warranted. Just like, are there any circumstances under which her alignment exercises aren’t enough and an external support like a pessary might be warranted for internal organ prolapse. TIA.
hahahahah, yeah I’ve had the exact same complaint. it frustrates me that she doesn’t communicate things very well but. I can share a little of what I’ve learned:
Firstly, you want to find out where your body alignment is currently at. And then bolster the parts that need it. However, the point of any crutch is to transition off of it. The arch in the foot is like a suspended bride, and the muscles are “suspended” but the strength and flexion capabilities are depended on the forces applied. That is, if the angel of the foot is turned out or in, the muscles that suspend, are not engaged, and the muscles become weak, because the body is very efficient in its use of all parts. If you don’t use it, you lose it.
Pelvic floor issues are complex, but for most, the issues stem from hamstring, adductor, and abductor shortened length and constant tucked or overly untucked pelves.
Imagine your body is like a robot’s body, it relies on a pulley system to move, walk, bend, lift etc. How you move, changes your muscles length, and then your muscles length changes your skeletal system, i.e. too tight or too loose, and then deforms the body like clay.
Many women have had problems with being barefoot anymore, because they only wore heels all day, and their hamstrings are so short that it hurts to have their heel on the ground. So they wear house shoes with heels. LOL.
Her exercises are actually enough, but I know its hard to follow because it involves learning about your body, which is important to learn, so you don’t injure yourself. There are so many yoga instructors too, that have knee and hip replacements, because all they were stretching were their tendons and ligaments, snd they stretched them so far that they are permanently hyper mobile in various parts of their body. Their form looked great, but they were actually injuring themselves more every day.
Finally, start with MOVE YOUR DNA. Its the best intro to her work, and the simplest to understand.
Also:
https://www.nutritiousmovement.com/stance/
https://www.nutritiousmovement.com/hypermobility/
https://www.nutritiousmovement.com/4-fast-fixes-for-pelvic-floor-disorder/
https://www.nutritiousmovement.com/ramblings-from-my-pelvis/
Her words and wisdom is unfortunately worth its weight in gold, but it does take effort to begin to understand. Try searching things with google like this:
Katy bowman hypermobility
That is literally th formula I used to find my pressing issues immediately because she explains and then gives an exercise. She also does have videos of her on-site classes (like $5 per hour vid, very much worth it!) that target direct issues.
https://www.nutritiousmovement.com/product/alignment-snacks-complete-set/
Lastly, I found her because I was hanging out with Japanese people all the time, and realized that they can squat with heels on the ground, and I couldn’t. Why? So I searched and searched and fucking searched the god damn internet, and only found stupid muscly men trying to explain how to deadlift. But then I found this : https://www.nutritiousmovement.com/you-still-dont-know-squat/
And she was the only person on the internet talking about it at the time. That’s why I respect her, even if she’s frustrating to understand sometimes. 🙂
Hope that helps. You can email me if you have further questions: kitsune (dot) sunday (at) gmail (dot) com. (obviously replace the dots with . ) 🙂
OH! and here’s this great post talking about how Kegals actually can cause PFD :
https://breakingmuscle.com/fitness/stop-doing-kegels-real-pelvic-floor-advice-for-women-and-men
Hi Kristen
What a fabulous article. Luckily, I do not suffer from any prolapses yet but, like you, wet myself a little when I sneeze or cough. What I am going to do is send your article to my sister, who is about to enter hospital for surgery on her cervix which has collapsed. She said she felt as though she had a badly inserted pessary (med) all the time. Thanks again for the article. Its great.
Nice to hear from you again! Tried most of what you wrote about including the electric toner at an actual physical therapist office. But after about seven years it has not been enough for me and I go in for my surgery in four days. I’ve had the good fortune of having some great Dr.’s and the only thing I can add to what you wrote is genetics. As a redhead, our fascia deteriorates more quickly than other people. As it deteriorates our organs continue to lose their fight with gravity and age.
This is SO IMOPORTANT! Thank you for being scared and doing it anyway. I just wanted to point to the difference between “normal” and “common”. The first refers to the way the body is supposed to be to function properly, the second refers to statistical prevalence. Upper spine curvature due to terrible posture and media device use is COMMON but not NORMAL. Pelvic disorders are also common but certainly NOT normal. Even doctors get this nomenclature wrong sometimes, but in this case the choice of words is very important.
Be well.
And check out Katie Bowman’s work. 😉
Thank you for publishing this. I have struggled with constipation since my second child was born. Like you, I use magnesium. I never required this before pregnancy. I’m wondering if analysis fissures are another symptom of anal prolapse? I bodybuild also so I am definitely engaged in daily exercices that would mitigate the problem. Any information you can send me, would be greatly appreciated
Excellent article! Thank you for all you shared to help other women.
Kristen, thanks for sharing. I had a VERY prolapsed uterus about 15 years ago after 3 kids and one very traumatic delivery. Anyways a few years after my third child, as you, being tired of not being able to jump on trampoline with kids, etc. I had surgery: partial hysterectomy and bladder sling and all has been good since (I am now 54), except my Urge incontinence is getting progressively worse. I did pelvic floor physical therapy which focussed on kegals with device and screen to monitor and coping strategies when the urge hits (eg counting backwards from 100 by 7s , etc). But only minimal help. I still dribble occasionally. Any thoughts on causes / cures for just Urge incontinence?? Thanks!!!!
If I were you, I would go to see a urogynecologist and ask them. It’s not uncommon for post-surgery women to experience prolapse again. It’s one of the reasons I would love to avoid surgery as long as possible (it’s often only temporarily effective). I’m not saying that’s what’s going on with you, but I would trust a urogynecologist to know!
Definitely look into homeopathy. A good constitutional remedy can inspire the body to heal itself in ways that seem miraculous, but really it’s how God designed our bodies. We are built for healing!
I second homeopathy. Sepia 200c taken once every 3 days helps heal uterus prolapse. Look up “Joette Calabrese Sepia”
Hi Kristen!
It’s so awesome you are bringing awareness to a very common (but as someone mentioned above not normal) issue that is not talked about openly enough, and many women suffer thinking they are alone and broken. I remember when things weren’t quite right anymore and feeling embarrassed, ashamed, scared, broken… I kept searching for answers after the doctors left me feeling worse… And then I came across Katy Bowman’s work and started to feel like there was hope, and then I also found Lauren Ohayon.
I highly recommend checking them both out, you won’t regret it ❤️
Thank you! This is very informative. I’ve been having some weird symptoms during the third trimester of my 4th pregnancy. I am going to look back into my Mutu account and will definitely go see a specialist post partum.
I really apreciate the way you share this oroblem. I am almost 80 years old, and is so difficult to convince people, that you are old but you can be healthier (if you tray), y leave in Mexico and most of the people having problems with pee just tell them, is normal and now you have to buy diapers o go for surgery. I have good results with electric accupunture, probably similar results with the kelger tonner. Thank you very much for your advice. Iwill tray pessari first.
Hi Kristin!
Thank You for your SUPER website!
Your articles are so GREAT & INFORMATIVE!
God Bless You & Yours!
A Greatful Fan,
Suzanne Jones
Bravo, for being vulnerable and providing well need information for all woman. I am a pelvic floor therapist and so many woman suffer in silence as if this is normal process without recourse. You did an excellent job in providing information as well as viable options for woman! Thank you.
Great article. I really wish you’d mentioned physical therapy in here as the first step. Kegels are not enough. You need someone trained to help you engage your entire pelvic floor. I went to PT after each of my kids was born and was amazed at how little i knew about relaxing and engaging my pelvic floor. The Vagina Whisperer is my favorite pelvic floor PT on instagram.
Hello kirstin,
I love all the work that you do! I’ve just found out I have multiple prolapses as well. I just had my 3rd baby a few months ago and I am 33 years old. This article was written about one year ago – do you have any updates? How are you feeling now? I’ve just started physical therapy and am working on my posture and just bought the K Ft exerciser like you recommended. I hope you are doing better! Like you, I want to avoid surgery also.
I’ve had a simple round pessary in for about a month, I’ve noticed increased back pain, mostly on the right side and growing. I lift a 7 mo old all day and figure menopause and lifting probably are contributing factors to the prolapse
Thank you for sharing your experiences and for your research. Your information has helped me immensely and I now am doing MUTU and have added the use of a kegel toner apparatus. I have a new found hope that I can get back to a modified “normal” lifestyle.
I knew I had a prolapse when I went for my annual OB appointment last year but was told it was stage 1 and nothing to worry about. If I wanted to do kegels that couldn’t hurt. Now I’m at stage 3, severe POP with bladder, rectal and uterine prolapse! I am 38 and pretty angry about what I was told by my OB, who otherwise is amazing. I also have a history of diastasis recti, which I did PT for and was told once that healed I could return to regular exercise – how I wish I had known not to! Anyway, all that to say thanks so much for this article! It’s given me hope that surgery isn’t my only option and I’ll be better informed when I meet with the specialist.
Check out cantienica method. Its THE solution fo prolapse
…And katy bowman.